The recovery model is playing a key role in these changes and advancements, becoming the standard mental health care model. Why should mental health care providers shift toward the recovery model and its values? How does it differ from traditional help?

What is the Recovery Model?
We understand that each person is unique and should seek support tailored to their needs. The recovery model is a relatively new, holistic mental health care approach based on two premises:
- Recovering from a mental health condition is possible.
- The best and most effective recovery is person-centred.
The concept of recovery includes the principles of hope, dignity, self-determination, and responsibility. These are the key components in treating people with mental health conditions through this model. This process aims to help people work beyond their limitations and encourage them to reach their full potential. Still, it is important to note that recovery can mean different things to different people.
Often, the recovery model is associated with the AA model and addiction recovery; currently, however, it is the path forward for all patient-centred mental health care in Canada. Endorsed by the Mental Health Commission of Canada (MHCC), Canadian Mental Health Association (CMHA), and the Centre for Addiction and Mental Health (CAMH), the values and principles of this approach are now known to most practitioners. However, fully incorporating them into programs and treatments is still ongoing.
Just a few decades ago, it was believed that patients with mental health conditions, especially those with schizophrenia, schizoaffective disorder, and bipolar disorder, couldn’t live a full life or contribute to society in purposeful ways. Long-term research has proven this wrong. The main principle and message of the recovery model is that those living with mental illness — including serious mental illness — can lead meaningful and satisfying lives despite their challenges.
Substance Abuse and Mental Health Services Administration (SAMHSA) has created a useful visual representation of the recovery model to better understand this approach – find it here. Although the recovery model is based on the idea that each recovery is unique, evidence suggests some shared similarities in symptoms and experiences can be grouped into the “CHIME” acronym, the concepts of which are explored in this diagram.
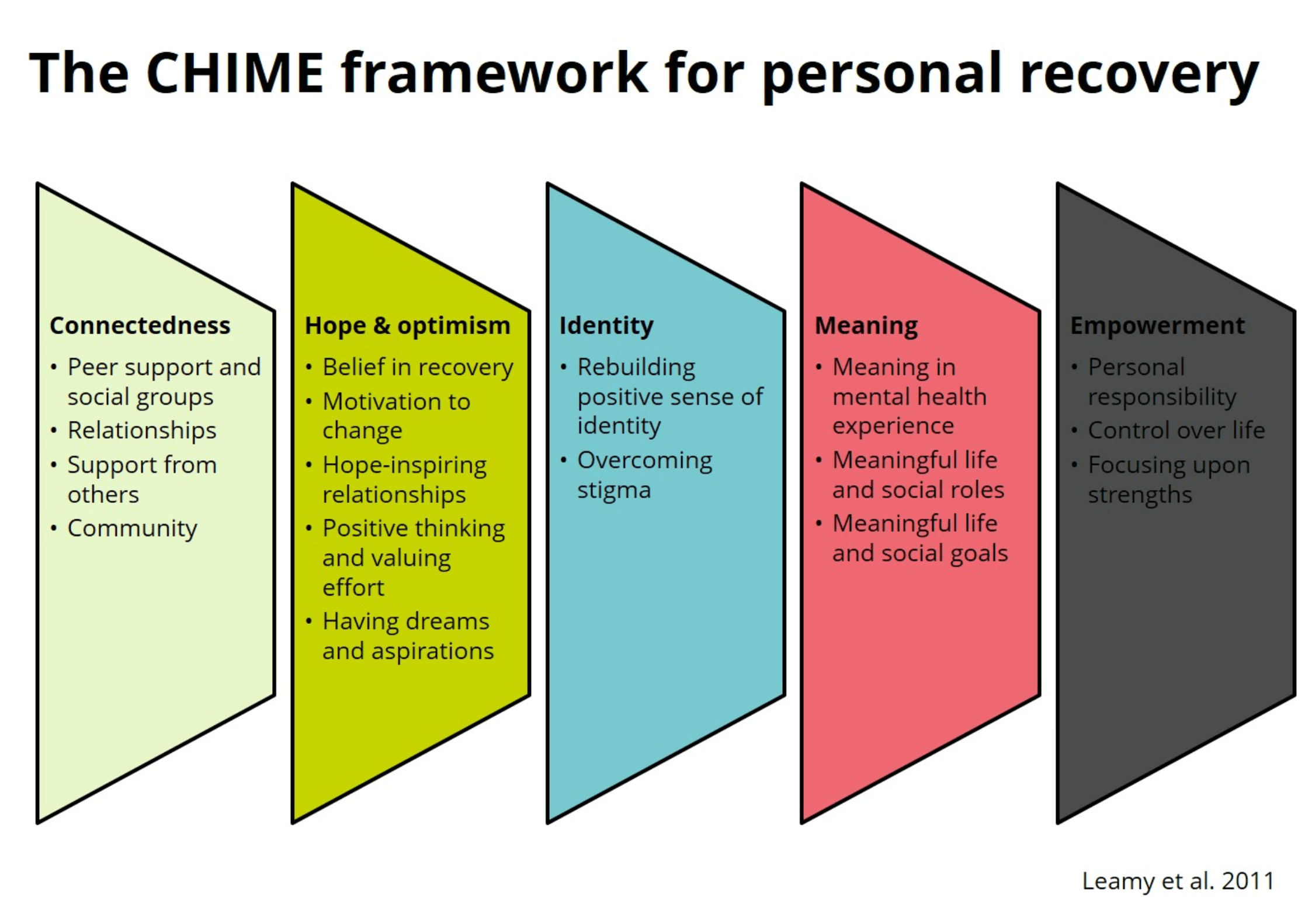

The Difference Between Models
The recovery model contrasts with the traditional model (also known as the medical model), which is based on the idea that mental disorders have physiological causes and, therefore, should be treated with medications. Unlike the medical model, the recovery model takes a more holistic approach and provides personal empowerment and peer support to those in need. The traditional model, however, is primarily focused on treatments rooted in empirical research.
Another key aspect of the recovery model is the importance of connectedness and social support. With supportive relationships and unconditional love, people with mental health conditions can better work through their symptoms, making the road toward recovery more manageable.
Although these two models are often presented as being at odds with one another, at Eli’s Place, we believe the best results can be achieved when both approaches are used in combination. This combined approach is supported by research. If both methods are integrated carefully and with expertise, they can make a huge difference and impact, explains National Alliance on Mental Illness.

The Recovery Model in Canada
As noted in a recent article from the University of Toronto: “With its emphasis on hope, the Recovery Model holds promise as a foundational framework for providing services for emerging adults that meet their unique developmental needs.” However, despite the national policy promoting recovery-oriented care, the recovery model in Canada still hasn’t been fully realized. Focus has primarily been on adult mental health and little attention has been paid to implementing this approach in the care of emerging adults. At Eli’s Place, we hope to reduce this gap.
Our farm-based residential treatment centre will assist people between the ages of 18-35. Our individualized therapeutic approach will support clients as they learn the tools needed to live with hope and purpose. Find out more about our therapeutic model here.
Mental health care in Canada is moving in a positive direction largely because of the recovery model. To learn more and stay updated on the latest news, challenges, and triumphs in mental health care, bookmark and continue to visit our blog.

Eli’s Place Communications Team
Our Eli’s Place blogs are developed & written by the Eli’s Place Editorial Team — a collaboration between staff and volunteers committed to raising awareness about serious mental illness in Canada. We aim to inform, inspire, and engage with readers who care about mental health and recovery.









